Irritable Bowel Syndrome or IBS is a chronic relapsing and often lifelong disorder involving a collection of symptoms, which vary from person to person but generally include:
- Abdominal pain or discomfort
- Bloating or distension
- Wind or flatulence
- Change in bowel habit (Diarrhoea and /or constipation)
I like to think of what happens in our gut as a continuum from ‘normal’ function to severe problems and we all find ourselves somewhere on that line.
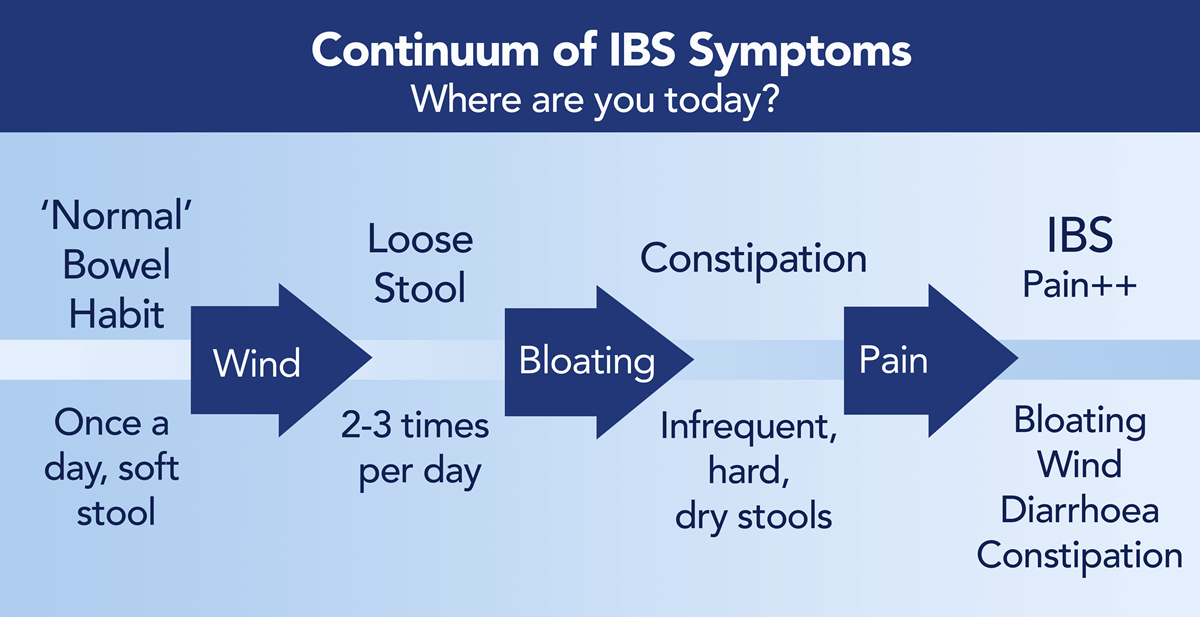
Who does IBS affect?
IBS most often affects people between the ages of 20 and 30 years and is twice as common in women than men. About 17% of people in the UK live with IBS, and many more probably have some symptoms but have never been to a doctor to talk about them. More recently it has been found to be present in older people too.
If your symptoms bother you often enough to disrupt your life, then you may have IBS.
What are the symptoms?
The symptoms can be catastrophic for many people and you may feel that you are not being taken seriously or that you are in so much pain that there must be something really wrong…you go back and forth to the doctor but nothing seems to work?
Also, the symptoms you experience may differ from day to day and not be the same as the next person with IBS, which makes it so difficult to diagnose.
Your first point of call should be your GP, as there is a set protocol for the GP to follow, which may require taking blood, or bowel sample to rule out other things, as some people with other gut disorders such as inflammatory bowel disease or coeliac disease have similar symptoms.
For this reason it is also difficult to perform research into the best diet for IBS.
Foods to Avoid when you have IBS
Most people report alcohol, caffeine and fatty foods as their IBS trigger foods.
More recently research has shown that some carbohydrates may contribute to IBS symptoms These carbohydrates are call Fermentable Oligo- saccharides, Di-saccharides Mono-saccharides and Polyols and a Low FODMAP diet to restrict them has grabbed media attention.
However rather than starting with a restrictive diet, some small changes may be all you need to control your symptoms and reduce the amount of medicines that you take. It is not advisable to commence a low FODMAP diet without the help of a registered dietitian – restricting your diet may mean that you avoid many foods and therefore miss out on some important nutrients which may lead to deficiencies. Also a healthy gut needs a variety of foods to keep the bacteria in balance.
Here are some things that anyone can try
- First find your IBS triggers – Keep a food diary!
- Eat regularly
- Drink enough fluid (8-10 cups of caffeine free drinks, non fizzy drinks or water)
- Chew your food well, and take time when eating.
- Reduce caffeine and alcohol.
- Try to reduce stress.
Keeping a Food and Symptom Diary
So keeping a food diary is a good way of helping you to notice the foods, which may upset you – it is important to carry the phone or paper you are using to note down with you rather than try and remember as it is easy to forget what you ate that day.
Below is an example of what to record, by reflecting on this and making small changes, you will find that over time your symptoms improve.
| Meal | Food eaten | Symptom |
| Breakfast 8am | White toast with butter -2 slices | – |
| Snack 11 am | Tea and 2 rich tea biscuits | – |
| Lunch | Nothing except water | – |
| – | – | 6.00pm pain and grumbling stomach |
| Evening meal | Curry with Friends | – |
| – | Chicken Tikka Starter, salad and dips | – |
| – | Dahl and Rice | 9.30pm Pain and wind, bloated – unable to sleep |
| All day -Coffee from machine at work | 5 or 6 cups | 11.30pm diarrhoea |
IBS Food Diary
[BBC:064] Food Diary
Keeping a food diary is a good way of noting which foods may upset you if you think you have IBS. This chart will help you keep a record of what you ate and when to identify triggers.
Eating Regularly
Sometimes we miss meals because we are in a rush or have pain and don’t know what best to eat. Planning ahead can help with this – if you already know what is less likely to cause you trouble, plan your meals around these foods, make yourself a sandwich the night before or keep a portion of last night’s meal to warm up for lunch the next day.
Fluids
Sometimes drinking more is just about reminding yourself – find something that you like to drink. Still water is best, so carry a bottle with you – aim to drink the whole bottle before you leave work or college or before say 6pm if you are at home that day.
Stress
Many people ask me “does stress really affect my gut?”
Well the answer is most definitely yes!
Think about people who get a bout of diarrhoea before an exam or interview…. this is part of our ‘Fight or Flight’ response, an innate system which prepares our body to face threat, such as a wild scary animal.
When we are stressed, our hormones prepare our body to fight or run away, this involves increasing our heart rate and our pulse and emptying our bowels… not very useful when facing an interview rather than a tiger!
However we can deal with this stress and help ourselves to relax. Try meditation, deep breathing techniques or using an app such as Calm or Headspace to talk you through a relaxation exercise. Physical Exercise also helps alleviate stress and improve mood, so try a walk, a swim, yoga or Pilates.
IBS and Caffeine
You may consider cutting down on caffeine and alcohol. Hopefully your food diary will have indicated how often you drink caffeinated drinks, How often do these appear?
- Cola, Diet Cola, Iron Brew
- Energy Drinks: Monster, Red Bull
- Tea
- Coffee – instant or freshly brewed
There are decaffeinated versions of many of these drinks so it’s an easy swap to change from normal coffee to decaffeinated and it doesn’t alter the taste too much. Most coffee shops will have decaffeinated versions too, you just need to ask when ordering. Some restaurants will have an alternative caffeine free drink such as mint tea, or other herbal varieties.
Most people find cutting down on alcohol a little more tricky. But it can be done! Try changing your drink to a single rather than a double, or swap to a low alcohol beer or wine. Try mixing them with lemonade or soda water to make a shandy or spritzer. Alternatively, choose a non-alcoholic drink every second round or try just slowing down so that you don’t drink as much in the same time frame. If you are thirsty try a non alcoholic drink to start with and remember to stick to no more than 14 units per week.
Fatty Foods and Fibre
Fatty foods are not great for anyone and therefore should be limited as part of a healthy diet. They also have been shown to aggravate some IBS symptoms such as diarrhoea.
High Fat foods include fried foods, many takeaway foods, pastries, crisps, cakes and biscuits; so try to limit your intake of these foods or choose a low fat variety.
I often say that Fibre is the only thing that you can eat more of! However it needs to be done with care as fibre can both improve IBS symptoms and make them worse.
Fibre is found in bread, rice pasta, fruit and vegetables, whole nuts and seeds. Try making small changes such as changing to wholemeal bread or white bread with added fibre. Wholemeal pasta and brown rice contain more fibre than the white varieties and wheat bisks, bran flakes and oats contain more fibre than cornflakes and rice krispies. You may wish to swap some of these, but don’t make too many changes at once as you won’t know what works and what doesn’t – I suggest starting with the thing you find easiest and leaving a week between changes.
Above all, it’s important to think about what you eat and listen to your body. Notice and record any changes to your symptoms as you make adjustments so that you learn what suits you. If you can follow the initial steps to drink plenty of water, eat regularly and avoid your triggers, you’ll then be able to take some additional steps towards a healthier and happier lifestyle. Reducing stress is never easy, but once you find something that works for you and your schedule, your belly will thank you for it!
Sarah Monk
Registered Dietitian

Hi I’m Sarah, a registered dietitian who currently works in a leadership role for the NHS. I became a dietitian because I love food, cooking and eating it… so what better job to do than talk about food all day!
I’m passionate about using food to help people feel better; I really do believe ‘we are what we eat’. However, changing what we eat is not as simple as swallowing a tablet and is a matter or trial and error and finding what’s right for you.










